Uterine Fibroids
Uterine fibroids represent the most common tumor in women in the reproductive age group.1 In around 50% of the patients, fibroids cause various symptoms, including abdominal pain and heavy menstrual bleeding.1 In some cases, uterine fibroids may even affect fertility and cause adverse pregnancy outcomes that include miscarriage.1,2
The techniques used to treat uterine fibroids are surgery, including myomectomy and hysterectomy, and non-surgical methods, like uterine artery embolization.1
Myomectomy Surgery: What is it
Myomectomy is a surgical procedure that removes uterine fibroids or myomas while preserving the patient’s child-bearing ability, unlike hysterectomy.3
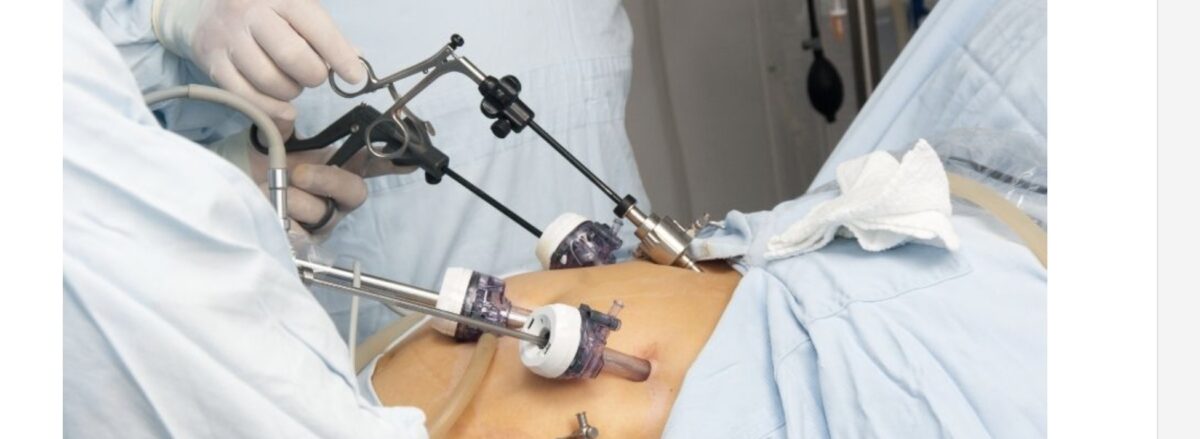
Three types of myomectomies are commonly used, namely, open abdominal, hysteroscopic and laparoscopic myomectomy.4,5 The choice of myomectomy depends on the size, number, and location of fibroids as well as personnel experience.4
It is not uncommon for a woman to undergo laparoscopic myomectomy and intra-operatively be converted to an open surgery due to the size or difficulty of removing the fibroids.
Myomectomy Surgery: Good Candidates
Women in the reproductive age group who wish to preserve their childbearing ability but are experiencing adverse symptoms of uterine fibroids are good candidates for myomectomy.4 Asymptomatic women in whom fibroids are increasing in size and are repeatedly causing miscarriage can also undergo this procedure.4
Pregnant women are generally not good candidates for myomectomy.2 However, they are eligible if they exhibit symptoms that conservative approaches cannot manage within 72 hours.2
Myomectomy Surgery: Risks
A critical risk of myomectomy is the high intraoperative bleeding, since tumors have their own vasculature and distort the anatomy.3 The risk of bleeding varies depending on the mode of surgery, as well as fibroid number, size and location.3 Bleeding results in adhesions inside the abdomen that cause the bowel to stick or twist around each other, this can result in obstruction in the future resulting in emergency room visits. Additionally, nearly 20% of the patients who go through myomectomy show the formation of adhesions inside the uterus.5 Such adhesions can result in abnormal menstruation and even infertility.6
It is not uncommon to require blood transfusions due to myomectomy-related bleeding.3
Other risks include surgical site infection, abscess, pulmonary embolism, and acute kidney injury within 30 days of the surgery.3
Furthermore, when pregnant women undergo myomectomy, they face a risk of complications, including uterine rupture, severe hemorrhage, preterm labor, and miscarriage.2
Myomectomy Surgery: Limitations
One of the most important limitations of myomectomy is that surgeons do not prefer to use it for removing more than three fibroids.11 This is not ideal for women that have numerous fibroids as there will be recurrent or persistent symptoms.
Another limitation of myomectomy is the need for reintervention in the years following the procedure. On an average, 19% of the patients who have undergone myomectomy are likely to require another intervention within five years of the procedure.7 However, this reintervention rate is still lower than that for other conservative treatments (24-33%).7
Another limitation is that surgeons cannot always palpate and remove small-sized fibroids during myomectomy, which can lead to recurrence.8
Myomectomy Surgery: Cost
The cost of myomectomy depends on the size and number of fibroids.9 For example, the cost of the procedure tends to be lower for patients who have larger fibroids than those with a greater number of fibroids.9 On an average, a myectomy could cost over $20,000 with hospital fees.9 There may be an additional expenditure of $9,800 for follow-up treatment over the course of four years after the procedure.9 There is also the additional cost for repeat or alternative treatment.
Myomectomy Surgery: Why it did not Work
There could be several reasons for why your myomectomy did not work for you.
The presence of more than two fibroids before the surgery is associated with fibroid recurrence.10 Similarly, child birth after the surgery increases the likelihood of fibroid recurrence.10 Another factor associated with recurrence is being over 36 years of age.10
There is also a chance that the surgeon was unable to palpate small fibroids and thus did not remove them.8 In such situations, the unremoved fibroids can grow and cause uterine fibroid-related symptoms to recur.8
While myomectomy can preserve fertility, it is also associated with various risks and limitations, depending on the patient’s specific condition. If you are a uterine fibroid patient, discuss the risks and limitations of myomectomy with your clinician before choosing a treatment.
UFE vs Myomectomy—Which is Right for You?
Far and away, the biggest difference between the two procedures is the degree of invasiveness.
With its increased level of surgical involvement, myomectomy carries an increased risk of infection, scarring, blood loss, and potential for reactions to the anesthetic used. There is also an increased risk of needing a complete hysterectomy. Recovery time can vary quite a bit—some patients have little post-op pain and can return to normal life within several days, but for others, a several week’s time is needed to recover.
Following a UFE, women are encouraged to limit their activities for 2-7 days to allow for healing. This includes avoiding heavy lifting and high impact exercise. Pain is generally minimal and most patients can get by with oral pain medication to manage it.
Depending on your type of fibroids, or the amount present, UFE may be preferable over myomectomy for women who wish to bear children in the future. Removing a large number of fibroids via myomectomy, for example, can negatively impact the entire uterine wall, leaving it unstable and prone to heavy bleeding. This can, in some cases, warrant a complete hysterectomy. Blood clots are also known to occur in higher frequency with a myomectomy procedure and in some cases the fibroid symptoms persist or return.4
UFE tends to be less impactful on the uterus without a need for stitches, minimal surgical scar, and negligible down time. The embolization of fibroids generally causes them to shrink permanently, and regrowth is rare.5
Some of the UFE advantages include:
- No hospital stay
- No general anesthesia
- No stitches
- No blood loss
- No risk of hysterectomy
- No major scars
- No surgical risks
How is the UFE performed?
- You will receive twilight sedation to help you relax
- Our specialist numbs the skin on the wrist or groin
- A tiny catheter is placed
- Small beads are placed into the fibroid artery
- The catheter is removed
- Band-Aid is applied
- Recover at home
We are Here to Help
Request an appointment to meet with our fibroid specialist who will review your imaging, labs and history to determine if you are candidate for the procedure, and the outcomes you can expect. Each woman is an individual and should discuss the potential risks and benefits of fibroid embolization and other treatments with our doctor to decide which option is best for her.
Appointments are available via an online video telehealth platform or in person at one of the offices in Los Angeles, Orange County or San Diego. Why should you choose us? Read here.
- Manyonda, I., Belli, A.M., Lumsden, M.A., Moss, J., McKinnon, W., Middleton, L.J., Cheed, V., Wu, O., Sirkeci, F., Daniels, J.P. and McPherson, K., 2020. Uterine-artery embolization or myomectomy for uterine fibroids. New England Journal of Medicine, 383(5), pp.440-451.
- Spyropoulou, K., Kosmas, I., Tsakiridis, I., Mamopoulos, A., Kalogiannidis, I., Athanasiadis, A., Daponte, A. and Dagklis, T., 2020. Myomectomy during pregnancy: A systematic review. European Journal of Obstetrics & Gynecology and Reproductive Biology, 254, pp.15-24.
- Kim, T., Purdy, M.P., Kendall-Rauchfuss, L., Habermann, E.B., Bews, K.A., Glasgow, A.E. and Khan, Z., 2020. Myomectomy associated blood transfusion risk and morbidity after surgery. Fertility and Sterility, 114(1), pp.175-184.
- Chen, R., Su, Z., Yang, L., Xin, L., Yuan, X. and Wang, Y., 2020. The effects and costs of laparoscopic versus abdominal myomectomy in patients with uterine fibroids: a systematic review and meta-analysis. BMC Surgery, 20(1), pp.1-9.
- Laganà, A.S., Garzon, S., Dababou, S., Uccella, S., Medvediev, M., Pokrovenko, D., Babunashvili, E.L., Buyanova, S.N., Schukina, N.A., Kaschchuk, M.G.S. and Kosmas, I., 2022. Prevalence of intrauterine adhesions after myomectomy: a prospective multicenter observational study. Gynecologic and Obstetric Investigation, 87(1), pp.62-69.
- Ma, J., Zhan, H., Li, W., Zhang, L., Yun, F., Wu, R., Lin, J. and Li, Y., 2021. Recent trends in therapeutic strategies for repairing endometrial tissue in intrauterine adhesion. Biomaterials Research, 25(1), pp.1-25.
- Davis, M.R., Soliman, A.M., Castelli-Haley, J., Snabes, M.C. and Surrey, E.S., 2018. Reintervention rates after myomectomy, endometrial ablation, and uterine artery embolization for patients with uterine fibroids. Journal of Women’s Health, 27(10), pp.1204-1214.
- Mukunda, S.B., Shen, Y. and Sugandha, S., 2019. Benefits and Limitations of Laparoscopic Myomectomy. Open Journal of Obstetrics and Gynecology, 9(03), p.292.
- Rana, D., Wu, O., Cheed, V., Middleton, L.J., Moss, J., Lumsden, M.A., McKinnon, W., Daniels, J., Sirkeci, F., Manyonda, I. and Belli, A.M., 2021. Uterine artery embolisation or myomectomy for women with uterine fibroids wishing to avoid hysterectomy: a cost–utility analysis of the FEMME trial. BJOG: An International Journal of Obstetrics & Gynaecology, 128(11), pp.1793-1802.
- Yoo, E.H., Lee, P.I., Huh, C.Y., Kim, D.H., Lee, B.S., Lee, J.K. and Kim, D., 2007. Predictors of leiomyoma recurrence after laparoscopic myomectomy. Journal of Minimally Invasive Gynecology, 14(6), pp.690-697.
- Conrad, D.H., Saar, T.D., Pacquée, S., Sarofim, M., Rosen, D., Cario, G. and Chou, D., 2018. Laparoscopic Myomectomy of a 4.2 kg Fibroid with Assistance of a Minilaparotomy. Gynecology and Minimally Invasive Therapy, 7(3), p.130.